our research
APPLICATIONS
Multimodal data integration for research and clinical applications.
Brain
Anti-angiogenic therapy monitoring in glioblastoma multiforme patients
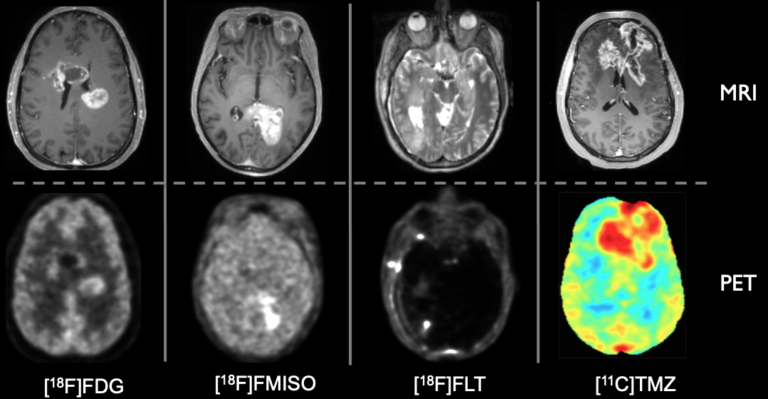
As part of an academic-industrial parternship brought together with the aim of using advanced PET/MRI for anti-angiogenic therapy monitoring in glioblastoma multiforme patients, an R01 project funded by NIH/NCI, we worked very closely with the engineers from Siemens Medical Solutions on improving the performance of the first human brain integrated PET/MR scanner so that the most advanced imaging studies can be performed using this device (Gerstner 2020).
Alzheimer's disease
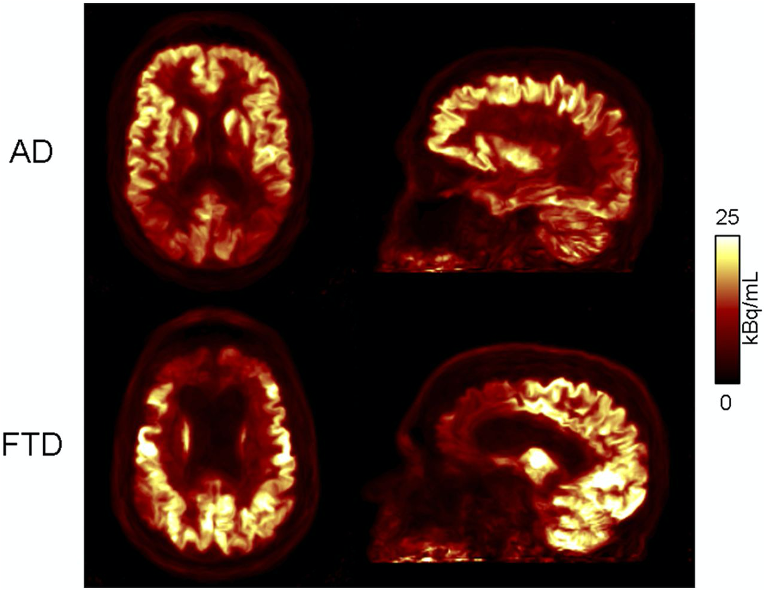
Funded by an R01 from NIH/NIBIB, we investigated the interrelation between structural, functional and metabolic changes in Alzheimer’s disease patients after MR-assisted PET data optimization. Reduced variability and increased SNR were observed after motion correction and anatomy-aided reconstruction. These results suggest PET data optimization may enable a more careful assessment of subtle changes in brain metabolism and allow for reduced sample sizes in future clinical trials (Chen 2018).
Cortical dopamine signaling and working memory
A study led by Dr. Joshua Roffman focused on better understanding schizophrenia, a devastating neuropsychiatric illness affecting approximately 1% of the global population and ranking among the top ten causes of disability in developed countries worldwide. The radiotracer [11C]NNC112 was used to study the distribution of cortical D1 receptor BP across network territories and to evaluate the relationship between D1 signaling and functional connectivity of working memory–related networks. This study specifically linked cortical dopamine signaling to network crosstalk that redirects cognitive resources to working memory, echoing neuromodulatory effects of D1 signaling on the level of cortical microcircuits (Roffman 2016).
Role of central dopamine in human bonding
In collaboration with Dr. Lisa Feldman-Barrett, we tested the role of central dopamine in human bonding. Our results suggest that synchronous maternal behavior is associated with increased DA responses to the mother’s infant and stronger intrinsic connectivity within the medial amygdala network (Atzil 2017).
Heart
Thrombus detection using [64Cu]FBP8
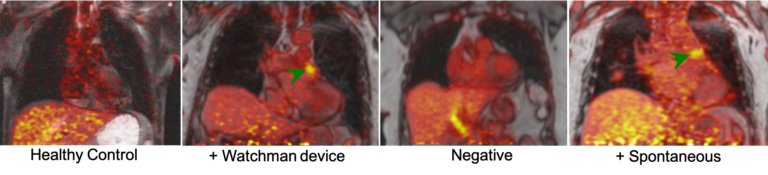
Working with Drs. David Sosnovik and Peter Caravan, we performed the preclinical and clinical studies aimed at assessing the value of [64Cu]FBP8, a novel fibrin-targeted probe developed in Dr. Caravan’s laboratory, for imaging thrombi in high-risk atherosclerotic plaque models and cardiovascular disease patients (David Izquierdo-Garcia et al 2020).
Measuring histone deacetylase (HDAC) levels using [11C]Martinostat
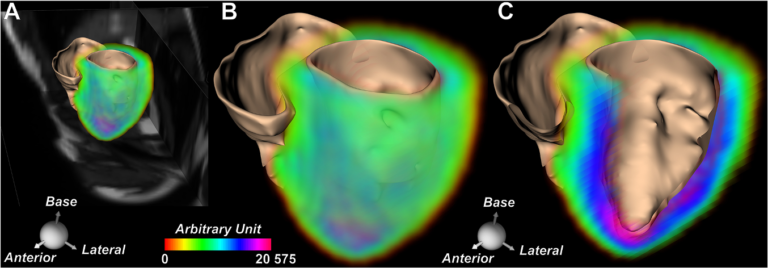
We collaborate with Dr. David Sosnovik to demonstrate that histone deacetylase (HDAC) activity in the human heart can be imaged in vivo using [11C]Martinostat, a class-1 HDAC-specific radiotracer developed in Dr. Jacob Hooker’s laboratory (David Izquierdo-Garcia et al. 2020).
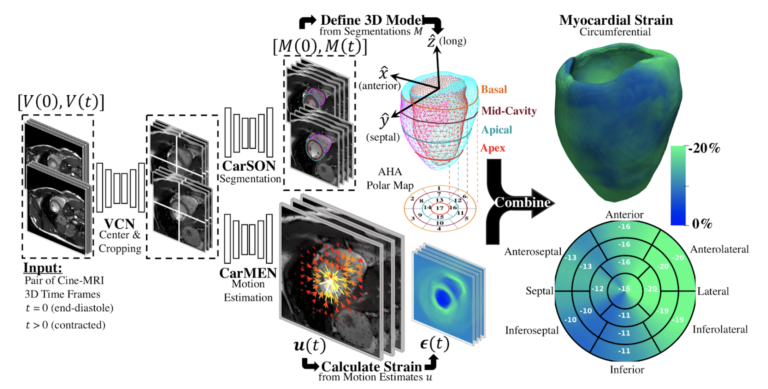
Deep learning-based myocardial strain estimation
The synergistic combination of various deep learning approaches we have developed for cardiac segmentation and motion estimation have enabled us to construct automated workflows for the global and regional characterization of cardiac mechanics (Manuel Morales et al. 2020).
In an ongoing collaboration with Dr. Niek Prakken (University Medical Center Groningen), we are assessing the value of DeepStrain in the detection of left-ventricular myocardial dysfunction in young overweigh, hypertensive and diabetic patients without history or knowledge of cardiac disease.
Lungs
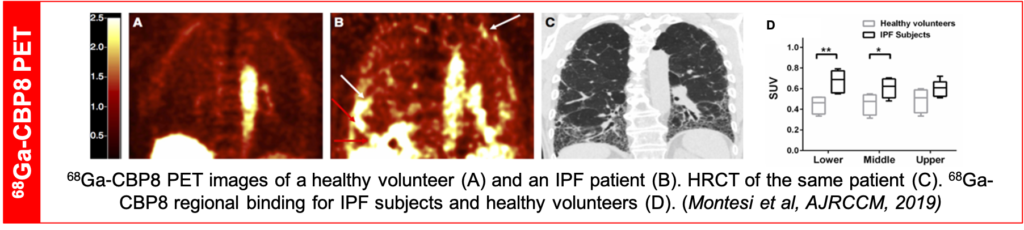
Fibrosis imaging in idiopathic pulmonary fibrosis using [68Ga]CBP8
A collaboration with Dr. Sydney Montesi led to the first-in-human studies using [68Ga]CBP8, a PET radiotracer that binds specifically to type I collagen developed in Dr. Peter Caravan’s laboratory, to assess safety and radiotracer distribution in healthy volunteers, and the ability to noninvasively measure increased lung collagen in subjects with idiopathic pulmonary fibrosis (Montesi 2019).
Liver
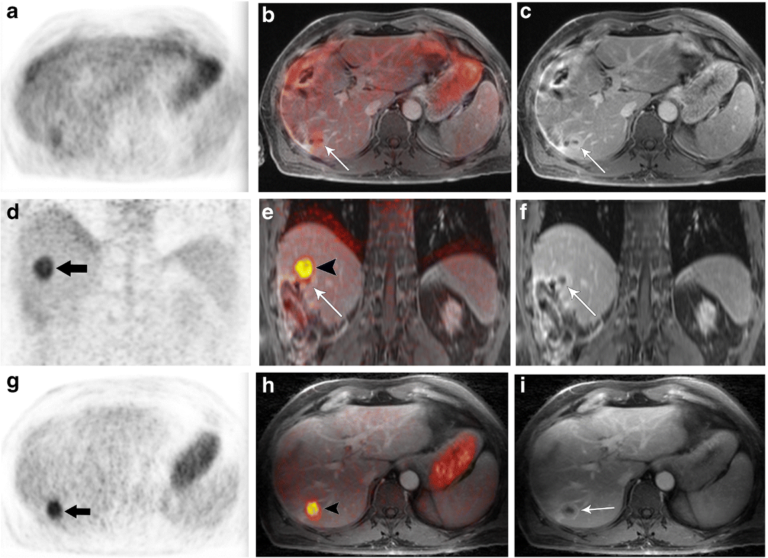
Clinical performance of motion correction for upper abdominal PET/DCE-MRI
After developing a novel self-navigated method that simultaneously corrects both PET data and DCE-MRI data for respiratory motion without increasing acquisition times, we focused on investigating its clinical performance and to compare the motion-corrected (MoCo) and uncorrected (non-MoCo) PET, MRI and fused PET/MRI data (Catalano 2018).
In this study, the quality of MoCo PET images was found to be higher than that of non-MoCo PET images. The improved quantitation allowed by MoCo PET might be clinically relevant. In fact, besides the contribution of PET quantitation to discriminating benign from malignant lesions, assessment of treatment response relies on measured differences in SUVmax and MTV along with possible complete visual disappearance of metabolically active lesions.
Furthermore, MoCo DCE-MRI might improve the overall quality of the data in patients unable to follow breathing instructions (deaf patients, patients with a different first language, or patients unable to hear the voice of the technologist while gradients are on), and in those with hemodynamic compromise in whom timing of arterial and portal venous phase imaging is challenging. The higher quality provided by fused PET/MRI data after MoCo has important clinical implications, as in the case of small but metabolically active lesions whose anatomic correlate might be difficult to identify. This is especially true when metabolic PET data are improperly fused over the MR anatomic overlay.
Hepatocellular carcinoma
In collaboration with Dr. Maria-Andreea Catana (BIDMC), we are investigating the utility of several radiotracers (e.g. [18F]DCFPyL, [64Cu]FBP8, etc.) in the characterization of hepatocellular carcinoma.